Painful diabetic peripheral neuropathy | JPR

Introduction
About 37 million people in the United States (US) have diabetes and as many as 96 million may have prediabetes.1 Diabetic neuropathy (DN) is the most common microvascular complication associated with diabetes. Diabetic peripheral neuropathy (DPN) affects about 50% of patients with diabetes,2 and symptomatic or painful DPN (pDPN) occurs in 30–50% of these patients.3–5 pDPN generally presents as a spontaneous burning pain of the feet, can be difficult to treat successfully, and has a significant impact on lifestyle and quality of life (QoL). The pathophysiology of pDPN is not well understood, but hyperglycemia-induced cellular damage in the nervous system results in hyperexcitable pain pathways, resulting in both peripheral and central sensitization.6 Thus, both primary afferent nociceptors and central neurons may contribute to neuropathic pain in pDPN.2,5
The management of pDPN is multifactorial, involving a combination of lifestyle factors (such as diet, exercise and weight loss) and pain medications. Because the pathogenesis of pDPN is poorly understood there is no mechanism-based approach to pharmacotherapy, resulting in doctors testing different treatments until something works.2,4 Glycemic control and risk factor management play an important role and, if well managed, can prevent or partially reverse DPN and modulate associated pain.6,7 There is a plethora of novel pharmacological agents that target a variety of pain pathways of potential therapeutic benefit in pDPN,7–9 although very few have gained FDA-approval for pDPN.2 Thus, the treatment of patients with pDPN is difficult, complex and frustrating for health-care professionals (HCPs), patients and caregivers.10,11
Whatever their diagnosis, patients are entitled to be informed about their condition and receive sound and clear advice about their treatment options. For patients with pDPN, the patient journey can consist of various stages: initially, because they may experience tingling and numbness, patients may not interpret what they feel in their feet as being pain, and this can delay the identification of foot pain; the search for information to obtain a diagnosis; the introduction of treatment; and thereafter, at any given time, evaluation of their current treatment, assessment of their current status (eg degree of ability/disability) and a review of their perspective of what the future holds.
The present survey was conducted to obtain information about the knowledge, experiences, emotions, and attitudes of patients with pDPN in the US, relating to their condition and their health care. The survey results will be used to investigate patient challenges, gaps in resources, treatment options, and to educate and equip patients with the information needed for them to become better advocates for themselves, as well as leading to more open discussion by patients about their pain and treatments.
Methods
Survey Method
This was a disease-level, patient-focused survey conducted in March 2021 as part of a program to increase awareness and discussion about pDPN in the US, leading up to National Neuropathy Awareness Week. The goal of the survey was to assess how to streamline the path to diagnosis and better disease management. To ensure credibility, relevance and resonance within the medical and patient advocacy community, the questionnaire was developed and conducted by SMS Research Advisors in collaboration with The Foundation for Peripheral Neuropathy and Averitas. Prior to conducting the survey, the questionnaire was reviewed by Averitas (legal, medical and regulatory review) and reviewed/validated by The Foundation for Peripheral Neuropathy. Averitas was not identified as a sponsor.
This qualitative market research study was conducted according to the ISPOR Code of Ethics.12 Clinical Research Ethics Committee or IRB approval for this type of qualitative market research is not required.
All respondents were screened against the following criteria, and only those fitting all the criteria (based on the information provided by each patient) were allowed to take the survey:
- Age 18 years or older,
- Diagnosis of diabetes with pDPN for at least 6 months,
- Receiving a prescribed treatment from a physician for their diabetic nerve pain for at least 6 months.
Respondents were recruited from a general population sample across the US (SMS Research used a third-party company and, where necessary, advocacy groups, to identify potential respondents) and the survey was conducted via an online questionnaire with an anticipated duration of 12–15 min.
Survey Design
The online questionnaire had three sections.
The first set of questions (S1 – S8) were “screening questions” to ensure participants met the desired profile based on the selection criteria. These questions covered the age of the participant, a diagnosis of diabetes (and the type), whether they currently experienced nerve pain due to the diabetes, the location and severity of their pain, how long since their first diagnosis of diabetic nerve pain of the feet, whether or not they were being treated for the pDPN and, if so, that this was with more than over-the-counter pain medication.
The second set of questions (Q1 – Q31) represented the full survey questionnaire from which desired patient insights would be derived. The full list of questions is presented in Table 1. The options for the types of pain that could be selected (Question 3) were as follows: a burning sensation, a painful cold, a pain like electric shocks, tingling, like touching pins and needles, numbness, itching, loss of sensation in the area, pain so significant that it interfered with daily activities. The information sources that could be selected (Question 6) included a range of HCPs and healthcare associations and organizations, other patients, family and friends, the internet, social media, pain medication manufacturers, advocacy groups and advertising in its various forms. Options that could be selected for responding to the question about reasons for changing medication (Question 15) included: increased severity of symptoms, wanting to try a new drug, lack of effectiveness, QoL (related to side effects) and medication not covered by health insurance.
 |
Table 1 Survey Questionnaire Questions Relating to Patient Insight |
Supplementary treatments that could be considered (Question 19) were diet, exercise, vitamins and supplements, medical marijuana, pain medications prescribed for other illnesses, complimentary or alternative treatments, alternating heat and cold, avoidance of use or contact when the pain is bad and distracting. Options that could be selected for challenges to seeking prescribed pain medication (Question 20) were diverse, including insufficient pain, stigma associated with drug use, fear of addiction, cost, inadequacy of dosage, poor past experience, too busy or too difficult to get to the doctor, concern about wasting the doctor’s time, concern that the doctor would not take the patient’s symptoms seriously, fear of talking about pain medications, risk of side effects or drug interactions, fear of more tests, already overmedicated, concerns about impact on QoL. Patients were asked which of the following activities they could no longer perform (Question 23) or they wished they could perform (Question 24): driving, travel, need to rest, use of walking aids, visiting family and friends or socializing, ability to work, use of sleep medications, reliance on caregivers and engagement with exercise.
In Question 28, patients were asked who they trust most to give the correct information about their diabetic nerve pain (selecting only one): primary care physician, diabetes specialist, pain specialist, podiatrist, neurologist, pharmacist, alternative or functional medical specialist, friend/relative, another patient, search engines, specific websites, online patient forums or social media.
The final group of questions (Q32 – Q44) were general demographic questions. Patients were asked their gender and ethnicity; if they lived in an urban, suburban or rural location; which state they live in; what level of education they had completed; whether they have children and, if so, what age; their current marital status; the number of people in their household; the household income; and whether they receive any disability allowance.
No personally identifiable information was requested, captured or stored during the survey.
Statistical Analysis
Due to the qualitative design of this market research survey, no formal statistical analyses were conducted. Data generated from the survey are presented as the proportion of individuals providing responses to each survey question.
Results
A total of 3636 adults started to respond to the survey (screening questions). The survey was completed by 506 adults who had diabetes were diagnosed with pDPN affecting the feet for at least 6 months, and who had received a physician-prescribed treatment for at least 6 months.
Demographics and Medical Condition
Overall, 79% of respondents had type 2 diabetes, 60% were male, and 70% were aged <65 years. 82% were Caucasian, 6% African American, 6% Hispanic, 3% mixed race, 2% Asian American, and 1% other ethnicities. 60% of respondents were married, 7% were in other committed relationships, 14% were single, 11% divorced or separated, and 8% widowed. 59% had undertaken tertiary education to degree level, including 7% with professional or advanced degrees.
In terms of household demographics, 17% of respondents lived alone, 30% were in a household of two people, 66% in a household of 3 or 4 people, and 13% in a household of ≥5 people. 57% had children in the household, mostly (82%) in the age 8–13 years. 61% of respondents lived in urban or suburban areas, and 39% in a rural area. 48% lived in a household having an annual income ≤US$50,000 and 18% were in a household with an annual income >US$125,000. The states having the highest number of participants were New York, California, Texas, and Florida.
Comorbidities were common among respondents; 13% of respondents had no comorbidity. Amongst those with comorbidities, 50% had hypertension, 38% obesity, 22% obstructive sleep apnea, 22% diabetic retinopathy, 16% cardiovascular disease, 12% chronic kidney failure and 11% hyperlipidemia. Osteoporosis, metabolic syndrome, autoimmune disease and nonalcoholic fatty liver disease were each reported in ≤9% of respondents.
Diabetes Pain Profile
In addition to foot pain, 50% of patients had pain in the legs and/or ankles, 40% had pain in the hands, 20% had shoulder pain and 2% had pain elsewhere. 37% of respondents had first been diagnosed with pDPN of the feet ≥3 years ago, whilst 25% had their first diagnosis 6–12 months ago. Pain was assessed as moderate (pain scale 3–6) in 50% of respondents, significant (scale 7–8) in 37% and severe (scale 9–10) in 12%. 66% had disability due to nerve pain. Pain medication was being taken daily by 48% of respondents and a couple of times per week in a further 37%.
The most commonly reported feelings respondents had about their nerve pain were as follows: “it makes me feel old” (44%), “it’s more of an annoyance than anything else” (42%), “I’m not sure what else I can do to help with the pain” (38%), “I’m increasingly unable to do things I want to do” (37%), “it hurts, but I have more important health issues to be concerned about” (33%) and “I’m worried I will lose my independence and need a caregiver” (30%).
Diabetes Symptoms and Diagnosis
In most respondents, the pDPN diagnosis was made at the time of diabetes diagnosis (19%) or later (60%); 17% of respondents received their pDPN diagnosis prior to being diagnosed with diabetes. The nerve pain was communicated to the doctor within 3 months of the patient first experiencing it in most cases (78%). Figure 1 shows the different types of pain experienced by respondents and the percentage experiencing each type. The most commonly reported pain types were `like touching pins or needles’ (58%), tingling (56%), and numbness (50%). In 30% of respondents, the pain was sufficient to interfere with the completion of daily activities.
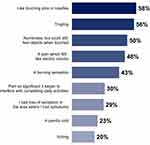 |
Figure 1 Type of pain experienced by respondents. |
As shown in Figure 2, the majority of patients (61%) took 2 or more doctors to receive a correct diagnosis, whereas 39% of respondents had their diabetic nerve pain correctly diagnosed by the first doctor they consulted; for 18% of respondents, it took visits to 3 or more doctors to get a correct diagnosis. Most respondents (56%) were very comfortable talking with their doctor about the pain in their feet, whilst 23% were somewhat comfortable and 22% were not comfortable 85% of respondents considered their conversations with their doctor about the pain in their feet to be “great” or “good”, and that the doctor clearly or generally understood the impact of the pain on their life. 12% of the respondents were frustrated that their doctor, whilst understanding the condition, was of limited or no help in managing the pain.
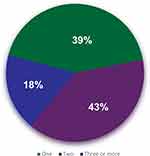 |
Figure 2 Number of doctors visited before a correct diagnosis of diabetic nerve pain was made. |
Treatment Aspects
Figure 3 presents the percentages of respondents reporting the previous (Figure 3A) and current (Figure 3B) use of different treatments. Anticonvulsants and over-the-counter pills and supplements were the most commonly used treatments, both previously and currently, with diet and exercise also playing significant roles. Prescribed topical creams and patches were currently used by 23% of respondents, an increase over what had been prescribed previously (15%). Similarly, the percentage of respondents receiving prescribed antidepressants was higher currently than in the past (22% versus 14%, respectively).
 |
Figure 3 Previous (A) and current (B) treatments. |
Since their initial diagnosis of pDPN involving the feet, 70% of respondents had taken ≥2 medications for the pain (33% had taken ≥3 medications). The reason for switching was a lack of effectiveness in 58%, worsening symptoms in 49% and declining QoL (generally too many side effects) in 46%.
A majority of respondents were not satisfied with their current treatment plan for their nerve pain (Figure 4). Amongst the 58% of respondents in this unsatisfied category, two-thirds were looking for greater pain relief and almost half for longer pain relief.
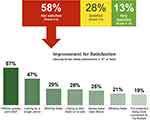 |
Figure 4 Overall treatment satisfaction (Question 16) rated on a scale from 0 (not enough pain relief) to 10 (pain successfully managed). |
When asked about their challenges in seeking prescribed pain medication for their pDPN (Question 20) respondents most commonly reported that they: are already taking a lot of medications and did not want to add more (32%), were worried about the potential for more side effects (31%) or were afraid of the impact on their QoL (23%), of interaction with their other medications (22%) or that they would become addicted to the pain medication (22%). 13% said that the out-of-pocket expense was too high and 10% were concerned that the medication would not be covered by their insurance. Statements relating to a negative relationship between a respondent and their doctor were reported by relatively few respondents, eg, that the respondent was wasting the doctor’s time (13%), that the doctor did not focus on their pain issue (10%) or that the doctor did not take their pain symptoms seriously (9%).
Knowledge and Sources of Information
66% of respondents reported that they understood more than just the basic facts about their pDPN involving the feet or had a solid understanding. 29% said that they knew only the basic facts and 5% did not know anything.
By far the most popular source of information about their pDPN was a medical professional (62% of respondents; Figure 5). The most common type of physician that respondents saw for their foot pain was a podiatrist (29%). The American Diabetes Association was by far the most utilized advocacy group for more information (36%). The most trusted sources for information about pDPN were also medical professionals (primary care physician, diabetes specialist physician, pain management physician, neurologist or podiatrist/hand specialist) in 74% of respondents. However, only 26% of respondents recorded their primary care physician as the most trusted source.
 |
Figure 5 Primary source of information for respondents about their diabetic nerve pain (Question 6); including only sources reported by ≥10% of respondents. |
70% of respondents had no difficulty finding the information they wanted about pDPN, and only 10% found it very difficult. Among those who found it difficult (scoring ≥6 on the 10-point difficulty scale), 41.1% found the information too scientific or academic, 31.9% said that their HCP did not believe that their foot pain was related to their diabetes and 30% reported that their HCP knew very little. Despite this, 64% of respondents indicated that their doctor was the person they felt best understood their pain and its impact on their life, followed by their spouse (41%).
Figure 6 presents the types of information that respondents found most valuable. Information about medications to treat or manage pain was reported to be the most valuable (58%), followed by information about the causes of pain (42%); approximately one-third of respondents reported that information about ideas on how to cope or deal with pain was valuable and a similar proportion reported that information about activities used to alleviate pain was valuable.
 |
Figure 6 Types of information reported as most valuable by respondents (Question 7). |
Attitudes and Behavioral Changes
When asked which four emotions respondents felt in a typical day since their diagnosis of pDPN involving the feet (Question 29), the top four emotions reported were all negative: frustrated (46%), worried (33%), anxious (26%) and uncertain (26%). Isolation, hopelessness, anger and fear were each reported in 19–20% of respondents. 22% of respondents recorded that they felt hopeful, 21% determined, and 14% in control.
The attitudes of respondents to their diabetic nerve foot pain were assessed in Question 30 of the survey in which they were asked to rate, on a scale from 1 (do not agree at all) to 10 (completely agree), how much they agreed or disagreed with a list of statements. The statements and the percentage of respondents reporting a score of 9 or 10 on each are presented in Figure 7. Overall, respondents felt relatively comfortable talking about their diabetic nerve foot pain and were actively seeking a remedy for their pain. The frustration highlighted in the emotional assessment was supported by higher percentages of respondents eager to find new medications to relieve their pain, desperate for a cure and wishing they could find the right tools to better understand their condition.
Figure 8 shows the lifestyle changes respondents reported as a result of their pDPN (Question 23). Most commonly, as a result of their pain, respondents reported the need to rest more often, stop or reduce physical activity, take more medications for their pain and to get to sleep. Respondents who indicated that they had made a change in their activities because of their pain were asked what they wished they could do more of. 31% wished they could engage in more physical activity, 28% that they could be active longer without rest, 20% that they could travel or participate in general entertainment, 20% that they did not need sleep medications and 20% that they spent less time lying in bed. Only 13% wished they could work more often.
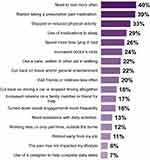 |
Figure 8 Lifestyle changes resulting from diabetic nerve pain (Question 23). |
33% of respondents did not currently use a primary caregiver, 43% had their spouse or partner as a primary caregiver, 16% had a friend or relative and only 7% relied on a home health aide. Amongst those requiring a caregiver, the activities for which help was most commonly required were as follows: preparing food (37%), walking (36%), transportation (35%), bathing/showering (33%), getting in and out of chairs (23%), dressing (22%), getting in and out of bed (22%) and eating/drinking (18%).
Future Outlook
The final survey question (Question 31) asked about future expectations. The results are shown in Figure 9. Better treatments (71%) and freedom from pain (61%) were the overriding perspectives among respondents when thinking about the future. Expectations about additional financial support or less skeptical doctors were only shared by about one-third of respondents (32% and 31%, respectively).
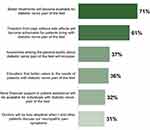 |
Figure 9 Future expectations of patients with diabetic nerve pain of the feet (Question 31). |
Discussion
The results of our online survey provide valuable qualitative information about the knowledge and experiences of 506 diabetic adults with pDPN in the USA. The high percentage of type 2 diabetics among respondents in the current study is consistent with other reports. In an observational study in England involving 15,692 diabetic patients, painful symptoms were present in 34%, with a diagnosis of pDPN in 21%. Painful neuropathic symptoms were twice as common in type 2 compared with type 1 diabetics.3 In that study, the risk of painful symptoms was 50% higher in females than males,3 whilst in a 2012 survey of patients with diabetes and symptoms of DPN (n=1004) in the US, 53% were female.13 The current survey included a higher proportion of males than females (60% vs 40%), indicating that the prevalence of pDPN may have been slightly under-represented compared with earlier studies.
The current survey also had a very high prevalence of Caucasian respondents (82%). This may have no reflection on the actual incidence of pDPN across ethnic groups. A study of the characteristics of pDPN symptoms in a multicultural population in the US had to use oversampling of Hispanics and African-Americans to recruit sufficient subjects, compared with Caucasians.14 Fewer Hispanics and African-Americans are diagnosed with pDPN in the US, possibly because of differences in perception of pain, but also because these patients are less willing to discuss pain, and generally less comfortable communicating, with their HCP.14
There may be a combination of reasons why many patients receive their diagnosis of pDPN after their diabetes diagnosis, including the subjective language patients use to describe their pain, some of which may not fall within the classic terminology for pDPN; a hesitancy of some patients to talk to their doctor about pain; the availability of too much information, with some sources not making the connection between foot pain and diabetes. In a community-based, cross-sectional study in type 2 diabetics in Taiwan (n=628), it was found that 30.6% had pDPN, but the primary health-care providers had paid little attention to pain symptoms or their treatment.15 In the US, a survey of patients with diabetes and symptoms consistent with DPN identified that, whilst 83% of the 1004 patients reported pDPN, only 41% had been diagnosed with DPN. 64% of HCPs never had patients complete DPN assessment questionnaires and did not perform specific diagnostic tests. Whilst 85% of patients reported that the pDPN impacted their daily life, their HCPs estimated that only 41% actually experienced pain and 38% had their daily life impacted.13
pDPN is associated with a substantial burden to patients, causing moderate-to-severe pain, which is often sub-optimally controlled, requiring polypharmacy, limiting physical activities and being associated with low levels of treatment satisfaction.16 Most patients genuinely struggle with finding a lasting solution to their pain. Despite most respondents in the present survey having tried two or more medications for their pain management, 58% remained unsatisfied with their treatment. Patients try multiple treatments, yet nothing seems to alleviate their pain. The lack of effectiveness could be because they are not just looking for a solution to their pain, but a solution to improving their lives. Patients tend to find temporary relief with one medication, then seek another treatment once the current treatment becomes ineffective (only 12% of patients in this survey stuck with the same treatment for a prolonged period). This is consistent with reviews of the literature which highlight the complexity of pharmacotherapy for the management of pain in pDPN patients.2,8,10
The language gap between laypersons (health consumers) and HCPs has long been recognized as a major barrier to effective health communication and health information comprehension.17 A recent study demonstrated that differences exist among health consumers with respect to the complexity of their language use when discussing health-related topics.18 A US survey of >1000 adults diagnosed with type 1 or type 2 diabetes who self-reported symptoms consistent with DPN concluded that, among patients and HCPs, misperceptions exist on the cause and management of pDPN, with additional disparities between the perspectives of patients and HCPs.13 The outcomes from that survey suggested a need for pDPN educational initiatives that target patients and HCPs, and the initiation of improved dialogue between patients and their HCPs for discussing appropriate management of pDPN that is distinct from treatment of the underlying diabetes. Nevertheless, in terms of access to information in the current study, most respondents reported that they knew what information they wanted (medication solutions), had no difficulty finding it and felt well-informed about their condition. This most likely reflects increased access to the internet globally, with 4.8 billion internet users as of January 2021,19 and the growing e-patient phenomenon.20 Moreover, 85% of respondents reported having great or good conversations with their doctor who they felt understood their pain and its impact on their life, possibly reflecting a sample bias due to the fact that most of the survey population was Caucasian with apparent good access to HCPs and information. However, for some patients there may be a lack of clear communication with their doctor, manifesting as a lack of trust in the doctor, and this may be a barrier for these patients. A significant disconnect in the doctor–patient relationship is highlighted by the finding that 64% of patients believe their doctor best understands their pain but only 26% mention their primary care physician as the person who they trust knows the most about their diabetic foot pain. This possibly suggests that while the doctor is sympathetic to the patient’s pain, they are not necessarily trusted to alleviate (or cure) the pain. Trust is the keystone of the patient-physician relationship and communication is fundamental to engendering trust.21–23 Effective communication improves satisfaction among patients and physicians, and patient adherence to medication and treatment regimens, decreases the number of medical errors, patient complaints and medical negligence claims, and positively impacts the overall clinical, physical and mental health outcomes for patients.24,25 A lack of clear patient/doctor communication in some cases may be confounded by the fact that many patients (34% of respondents in this survey) know only the basic facts or nothing about their condition, and the high incidence of worry, frustration, anxiety, anger and lack of hope among some patients. These emotions may fuel an inability to interpret properly what is being said and make it difficult for doctors to tell their patients things they may not want to hear. As a result, patients can feel they are not “being heard” by doctors and doctors feel their patients “don’t understand” what they are trying to say. Again, this highlights the need for improved educational material to address communication and knowledge gaps. Patients with pDPN and HCPs have previously acknowledged the value of learning more about pDPN.13
Pain catastrophizing26 has been shown to be significantly associated with pain disability, QoL, and physical activity decline in patients with DPN.27 Furthermore, depression, anxiety, pain acceptance, pain severity and sleep disturbance are also predictors for a declining QoL in patients with DPN.28,29 A report by the Danish Center for Strategic Research involved a questionnaire on neuropathy and pain completed by 5514 patients with type 2 diabetes. The prevalence of possible DPN and pDPN was 18% and 10%, respectively, somewhat lower than has been reported elsewhere. However, both DPN and pDPN were associated with lower QoL, poorer sleep, depression, and anxiety.30 Mental, as well as physical function, is impaired in pDPN patients compared with these functions in diabetic patients without pain.31 Early and effective diagnosis and management of pain in patients with DPN is, therefore, important to try to avoid pain catastrophizing and the emotional and other factors associated with a decline in QoL. In our study, the most common emotions reported in a typical day were all negative: frustrated (46%), worried (33%), anxious (26%), and uncertain (26%), with approximately 20% of respondents each reporting feelings of isolation, hopelessness, anger or fear.
Consistent with reported practice, respondents in this survey focused on two different paths to pain management: lifestyle changes and medical treatments. Among lifestyle changes, diet, vitamins and exercise were most popular. Diet, exercise and weight loss can not only help with remission of diabetes but they can also reverse DPN.2 Most of the reported changes in lifestyle in the current survey related to the ability to perform physical activities, the need for more rest and problems with sleeplessness. A desire to still work was less frequently reported, perhaps partly accounted for by 30% of respondents being aged >65 years. Not surprisingly, spouses/partners were the most common primary caregiver, when required. Activities requiring prolonged periods of standing, such as walking and food preparation, were the activities that required the most assistance from a caregiver. Whilst some patients accept that they need to moderate their current lifestyle, others had an expectation of a complete cure with about one-third of respondents being desperate for a cure for their diabetic nerve pain. This may help account for some of the doctor/patient communication difficulties and negative emotional profiles reported in this survey.
Tricyclic anti-depressants, serotonin-noradrenaline reuptake inhibitors, anticonvulsants, opioids and topical treatments are the approved and most commonly prescribed medications for pDPN.2,32 Although the previous and current use of prescribed anticonvulsants was reported most commonly in our survey, over-the-counter pills and foot creams/patches were also reported to be used commonly among respondents. Other prescribed medications included antidepressants, creams, patches, and opioids, generally reflecting the approved medications for pDPN. Interestingly, compared with previously, approximately 30% more respondents reported the current use of prescribed topical creams and patches.
Patients primarily want to see a future where better treatments become available for pDPN of the feet. They also want to see a day when they can be free from the side effects associated with their pain medication. Approximately one-third of patients indicated they hope for greater awareness of pDPN, that access to education improves and doctors become less skeptical about patients with pDPN.
One approach to improving treatment satisfaction amongst patients with pDPN (at least amongst the one-third who feel under-informed) could be to make it easier for them to find information about treatments. This could involve helping doctors to create a more focused treatment plan, as well as improving information about the link between diabetes and nerve foot pain. Another factor could be educating physicians about treatment options, particularly regarding differences in adverse event profiles. Topical treatments are considered a good option for patients with pDPN who are intolerant to conventional systemic therapies due to an unwillingness to use them because of dependence concerns, or adverse events.2 Additionally, topical treatments significantly reduce the risk of drug interactions, which is particularly important in patients with multiple co-morbidities and those experiencing polypharmacy;2 indeed, polypharmacy can pose a significant risk to patient health (eg renal issues and fractures) in elderly individuals who are often prescribed numerous medications.33 In the present survey, topical patches and creams were currently prescribed to only 23% of respondents, while 19% used over-the-counter (OTC) topical creams or patches. Of note, although numerous OTC creams and patches are available, the capsaicin 8% topical system (Qutenza®) is the only HCP-prescribed topical treatment, and only topical formulation of capsaicin, approved by the US Food and Drug Administration (FDA) to treat pDPN of the feet.34 A network meta-analysis of 25 randomized, controlled clinical trials involving the capsaicin 8% topical system versus other treatments for pDPN showed that the patches had similar efficacy to oral agents with fewer side effects.35
By design, qualitative surveys of this nature present limitations.36 To avoid potential bias associated with using an organization’s membership sample, the survey was conducted using a “general population” sample of individuals. However, it is important to note that the study sample was mostly Caucasian, male, educated, and with a high prevalence of comorbidities. Therefore, our findings may not be generalizable to the broader US population with diabetes and pDPN of the feet.
Conclusions
People with pDPN affecting the feet commonly experience sharp or tingling pain, which can be severe and may impact their lifestyle and emotional well-being. They generally report pain to their doctors promptly but may need to see several doctors before receiving a correct diagnosis. Treatment is multifactorial, involving diet, exercise, lifestyle changes and pharmaceuticals. Most patients have tried multiple therapies, remain unsatisfied with their current pain treatment, and struggle to find a lasting solution for their pain. Patients seek information from various sources, but predominantly from HCPs. Most are comfortable communicating with their doctor and find the information they are looking for, but about one-third feel insufficiently informed. Early identification and diagnosis of pain in patients with diabetes, and education about pain treatments, is important to reduce or avert the impact of pain on QoL and emotional well-being.
Abbreviations
DN, diabetic neuropathy; DPN, diabetic peripheral neuropathy; FDA, Food and Drug Administration; HCP, health-care professional; OTC, over-the-counter; pDPN, painful diabetic peripheral neuropathy; QoL, quality of life.
Acknowledgments
The authors acknowledge Lindsay Colbert, Executive Director, Foundation of Peripheral Neuropathy, who reviewed the questionnaire and provided insights before execution of the project. Professional medical writing support was provided by Jon Monk and David P. Figgitt PhD, ISMPP CMPP™, Content Ed Net, with funding from Averitas Pharma (A Grünenthal Company).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
The research and survey were conducted by SMS Research Advisors with funding from Averitas Pharma (A Grünenthal Company). Panel respondents were compensated for their participation in the survey.
Disclosure
Alaa A Abd-Elsayed is a consultant for Medtronic, Avanos, Abbott, Sprint, and Averitas Pharma. Lizandra P Marcondes and Zachary B Loris are employees of Averitas Pharma (A Grünenthal Company). Dan Reilly was an employee of SMS Research Advisors. The authors report no other conflicts of interest in this work.
References
1. Centers for Disease Control and Prevention. The facts, stats, and impacts of diabetes. Available from: https://www.cdc.gov/diabetes/library/spotlights/diabetes-facts-stats.html#:~:text=Key%20findings%20include%3A,t%20know%20they%20have%20it.
2. Azmi S, Alam U, Burgess J, Malik RA. State-of-the-art pharmacotherapy for diabetic neuropathy. Expert Opin Pharmacother. 2021;22(1):55–68. doi:10.1080/14656566.2020.1812578
3. Abbott CA, Malik RA, van Ross ER, Kulkarni J, Boulton AJ. Prevalence and characteristics of painful diabetic neuropathy in a large community-based diabetic population in the UK. Diabetes Care. 2011;34(10):2220–2224. doi:10.2337/dc11-1108
4. Qureshi Z, Ali MN. Diabetic neuropathy pain management: a global challenge. Curr Diabetes Rev. 2021;17(5):e031120187542. doi:10.2174/1573399816666201103142521
5. Feldman EL, Callaghan BC, Pop-Busui R, et al. Diabetic neuropathy. Nat Rev Dis Primers. 2019;5(1):41. doi:10.1038/s41572-019-0092-1
6. Veves A, Backonja M, Malik RA. Painful diabetic neuropathy: epidemiology, natural history, early diagnosis, and treatment options. Pain Med. 2008;9(6):660–674. doi:10.1111/j.1526-4637.2007.00347.x
7. Javed S, Petropoulos IN, Alam U, Malik RA. Treatment of painful diabetic neuropathy. Ther Adv Chronic Dis. 2015;6(1):15–28. doi:10.1177/2040622314552071
8. Rastogi A, Jude EB. Novel treatment modalities for painful diabetic neuropathy. Diabetes Metab Syndr. 2021;15(1):287–293. doi:10.1016/j.dsx.2021.01.004
9. Dewanjee S, Das S, Das AK, et al. Molecular mechanism of diabetic neuropathy and its pharmacotherapeutic targets. Eur J Pharmacol. 2018;833:472–523. doi:10.1016/j.ejphar.2018.06.034
10. Alam U, Sloan G, Tesfaye S. Treating pain in diabetic neuropathy: current and developmental drugs. Drugs. 2020;80(4):363–384.
11. Iqbal Z, Azmi S, Yadav R, et al. Diabetic peripheral neuropathy: epidemiology, diagnosis, and pharmacotherapy. Clin Ther. 2018;40(6):828–849. doi:10.1016/j.clinthera.2018.04.001
12. Santos J, Palumbo F, Molsen-David E, et al. ISPOR code of ethics 2017 (4th edition) – appendix 3. Value Health. 2017;20(10):1227–1242. doi:10.1016/j.jval.2017.10.018
13. Sadosky A, Hopper J, Parsons B. Painful diabetic peripheral neuropathy: results of a survey characterizing the perspectives and misperceptions of patients and healthcare practitioners. Patient. 2014;7(1):107–114. doi:10.1007/s40271-013-0038-8
14. Eichholz M, Alexander AH, Cappelleri JC, et al. Perspectives on the impact of painful diabetic peripheral neuropathy in a multicultural population. Clin Diabetes Endocrinol. 2017;3:12. doi:10.1186/s40842-017-0051-2
15. Jane SW, Lin MS, Chiu WN, Beaton RD, Chen MY. Prevalence, discomfort and self-relief behaviours of painful diabetic neuropathy in Taiwan: a cross-sectional study. BMJ Open. 2016;6(10):e011897. doi:10.1136/bmjopen-2016-011897
16. Gore M, Brandenburg NA, Hoffman DL, Tai KS, Stacey B. Burden of illness in painful diabetic peripheral neuropathy: the patients’ perspectives. J Pain. 2006;7(12):892–900. doi:10.1016/j.jpain.2006.04.013
17. Zeng QT, Tse T. Exploring and developing consumer health vocabularies. J Am Med Inform Assoc. 2006;13(1):24–29. doi:10.1197/jamia.M1761
18. Yu B, He Z, Xing A, Lustria MLA. An informatics framework to assess consumer health language complexity differences: proof-of-concept study. J Med Internet Res. 2020;22(5):e16795. doi:10.2196/16795
19. Internet Trends 2023. Stats & facts in the US and worldwide. Available from: https://www.vpnmentor.com/blog/vital-internet-trends/.
20. Gerber BS, Eiser AR. The patient physician relationship in the internet age: future prospects and the research agenda. J Med Internet Res. 2001;3(2):E15. doi:10.2196/jmir.3.2.e15
21. Pellegrini CA. Trust: the keystone of the patient-physician relationship. J Am Coll Surg. 2017;224(2):95–102. doi:10.1016/j.jamcollsurg.2016.10.032
22. Honavar SG. Patient-physician relationship – communication is the key. Indian J Ophthalmol. 2018;66(11):1527–1528. doi:10.4103/ijo.IJO_1760_18
23. Gu L, Tian B, Xin Y, Zhang S, Li J, Sun Z. Patient perception of doctor communication skills and patient trust in rural primary health care: the mediating role of health service quality. BMC Prim Care. 2022;23:255. doi:10.1186/s12875-022-01826-4
24. Anderson PF, Wescom E, Carlos RC. Difficult doctors, difficult patients: building empathy. J Am Coll Radiol. 2016;13(12 Pt B):1590–1598. doi:10.1016/j.jacr.2016.09.015
25. Tongue JR, Epps HR, Forese LL. Communication skills for patient centered care: research-based, easily learned techniques for medical interviews that benefit orthopaedic surgeons and their patients. J Bone Joint Surg Am. 2005;87(3):652–658. doi:10.2106/00004623-200503000-00027
26. Sullivan MJL, Bishop SR, Pivik J. The pain catastrophizing scale: development and validation. Psychol Assess. 1995;7(4):524–532. doi:10.1037/1040-3590.7.4.524
27. Geelen CC, Kindermans HP, van den Bergh JP, Verbunt JA. Perceived physical activity decline as a mediator in the relationship between pain catastrophizing, disability, and quality of life in patients with painful diabetic neuropathy. Pain Pract. 2017;17(3):320–328. doi:10.1111/papr.12449
28. Davoudi M, Rezaei P, Rajaeiramsheh F, Ahmadi SM, Taheri AA. Predicting the quality of life based on pain dimensions and psychiatric symptoms in patients with painful diabetic neuropathy: a cross-sectional prevalence study in Iranian patients. Health Qual Life Outcomes. 2021;19(1):49. doi:10.1186/s12955-021-01697-w
29. Kioskli K, Scott W, Winkley K, Kylakos S, McCracken LM. Psychosocial factors in painful diabetic neuropathy: a systematic review of treatment trials and survey studies. Pain Med. 2019;20(9):1756–1773. doi:10.1093/pm/pnz071
30. Gylfadottir SS, Christensen DH, Nicolaisen SK, et al. Diabetic polyneuropathy and pain, prevalence, and patient characteristics: a cross-sectional questionnaire study of 5514 patients with recently diagnosed type 2 diabetes. Pain. 2020;161(3):574–583. doi:10.1097/j.pain.0000000000001744
31. Gore M, Brandenburg NA, Dukes E, Hoffman DL, Tai KS, Stacey B. Pain severity in diabetic peripheral neuropathy is associated with patient functioning, symptom levels of anxiety and depression, and sleep. J Pain Symptom Manage. 2005;30(4):374–385. doi:10.1016/j.jpainsymman.2005.04.009
32. Khdour MR. Treatment of diabetic peripheral neuropathy: a review. J Pharm Pharmacol. 2020;72(7):863–872. doi:10.1111/jphp.13241
33. Rochon PA, Petrovic M, Cherubini A, et al. Polypharmacy, inappropriate prescribing, and deprescribing in older people: through a sex and gender lens. Lancet Healthy Longev. 2021;2:e290–e300. doi:10.1016/S2666-7568(21)00054-4
34. Averitas Pharma, Inc. Qutenza® (Capsaicin) Topical System: US Prescribing Information. Morristown, NJ: Averitas Pharma, Inc; 2022.
35. van Nooten F, Treur M, Pantiri K, Stoker M, Charokopou M. Capsaicin 8% patch versus oral neuropathic pain medications for the treatment of painful diabetic peripheral neuropathy: a systematic literature review and network meta-analysis. Clin Ther. 2017;39(4):787–803.e18. doi:10.1016/j.clinthera.2017.02.010
36. Queirós A, Faria D, Almeida F. Strengths and limitations of qualitative and quantitative research methods. Eur J Educ Stud. 2017;3(9):369–387.




